Biology
Microbiology
Immune System
Lymphatic Organs
Red Bone Marrow
Lymph Nodes
Thymus
Spleen
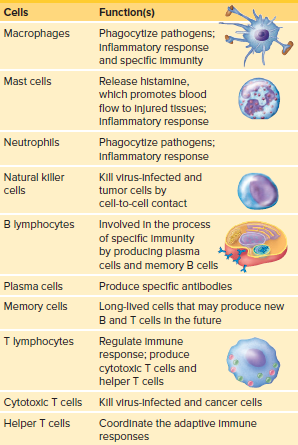
Cells of the Immune System
Nonspeciic Defenses
Innate Immunity
Inflammatory Response
Complement System
Natural Killer Cells
Specific Defenses
Adaptive Immunity
B Cells
Antibodies
ABO Blood Type
T Cells
Cellular Response
Helper T Cells
Tissue Rejection
Immunizations
Allergies
Autoimmune Diseases
AIDS
University/Undergrad

Chapter 26: Defenses Against Disease
26.1 Overview of the Immune System
The immune system fights infections and cancer to keep us healthy.
The immune system contains lymphatic organs such as the red bone marrow, thymus, lymph nodes, and spleen.
Lymphoid tissue can also be found in the tonsils and appendix.
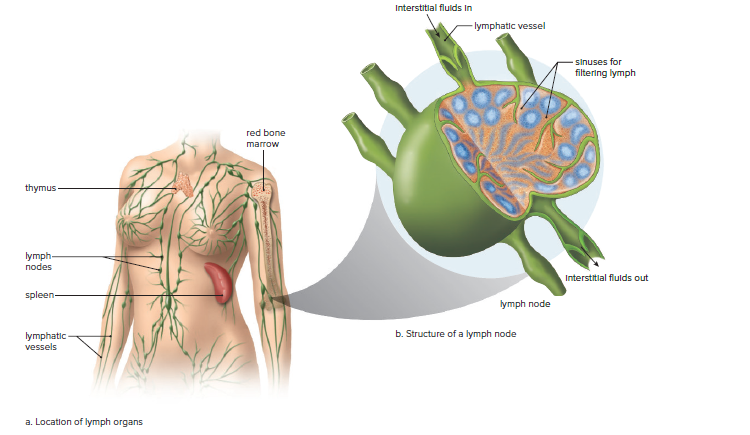
Lymphatic Organs
Each of the lymphatic organs has a particular function in immunity, and each is rich in lymphocytes, one of the types of white blood cells.
Red Bone Marrow
Most bones in a child have red bone marrow
In an adult, red bone marrow is still present in certain bones:
Skull
Sternum (breastbone)
Ribs
Clavicle
Pelvic bones
Vertebral column
Ends of the humerus and femur nearest their attachment to the body
Red bone marrow produces all types of blood cells.
Lymphocytes differentiate into B lymphocytes (B cells) or T lymphocytes (T cells).
B lymphocytes are produced and mature in the bone marrow.
T lymphocytes mature in the thymus.
B lymphocytes produce antibodies.
T lymphocytes kill antigen-bearing cells outright.
Thymus
The thymus is soft and bilobed.
The size of the thymus varies and is larger in children.
The thymus shrinks as we get older.
The thymus plays a role in the maturing of T lymphocytes.
Immature T lymphocytes migrate from the bone marrow to the thymus.
T lymphocytes mature in the thymus.
Only 5% of T lymphocytes leave the thymus.
T lymphocytes that react with our own body die.
T lymphocytes that can attack foreign cells leave the thymus and enter lymphatic vessels and organs.
Lymph Nodes
Lymph nodes are small, ovoid structures along lymphatic vessels.
Lymph nodes filter lymph and keep it free of pathogens and antigens.
Lymph is filtered as it flows through a lymph node because the node’s many sinuses (open spaces) are lined by macrophages.
Macrophages are large, phagocytic cells that engulf and then devour as many as a hundred pathogens and still survive.
Lymph nodes contain many lymphocytes and are instrumental in fighting infections and cancer.
Some lymph nodes are located near the surface of the body and are named for their location.
For example, inguinal nodes are in the groin, and axillary nodes are in the armpits.
Physicians often feel for the presence of swollen, tender lymph nodes in the neck as evidence that the body is fighting an infection.
This method is a non-invasive, preliminary way to help them make a diagnosis.
Spleen
The spleen is located in the upper left abdominal cavity and is about the size of a fist.
The spleen filters the blood and contains red pulp and white pulp tissue.
The red pulp sinuses filter the blood of pathogens and debris, including worn-out red blood cells.
The white pulp contains lymphocytes that fight infections and cancer.
The spleen's outer capsule is thin and can burst due to infection or severe blow.
Other organs can fulfill the spleen's functions, but individuals without a spleen are more susceptible to infections.
People without a spleen may need to receive certain vaccinations and antibiotic therapy indefinitely.
Other Locations of Lymphoid Tissue
Tonsils and the appendix are lymphatic tissue structures.
Tonsils are located in the pharynx.
The appendix is attached to a portion of the large intestine.
Both tonsils and appendix belong to the immune system.
Cells of the Immune System
The immune system consists of lymphatic organs, lymphatic tissues, and various cells.
The cells in the immune system help distinguish between self and nonself cells.
Pathogens are identified by the presence of antigens, which are usually proteins or carbohydrates.
The immune system provides immunity by repelling foreign substances, pathogens, and cancer cells.
There are two levels of immunity: nonspecific immunity and specific (adaptive) immunity.
Nonspecific immunity repels pathogens indiscriminately, while specific immunity requires a certain antigen to be present.
26.2 Nonspecific Defenses and Innate Immunity
The body has innate immunity.
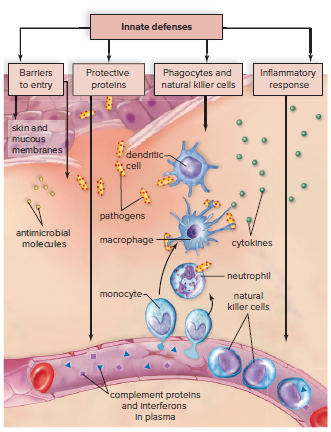
Innate immunity is composed of various types of nonspecific defenses.
Nonspecific defenses are the first line of defense against most types of infections.
Nonspecific defenses include:
Barriers to entry.
Inflammatory response.
Complement system.
Natural killer cells.
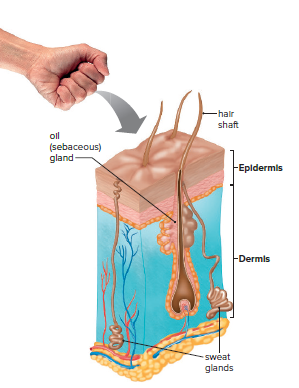
Barriers to Entry
Skin and mucous membranes in respiratory, digestive, reproductive, and urinary tracts act as mechanical barriers to pathogens.
Oil gland secretions contain chemicals that weaken or kill certain bacteria on the skin.
The upper respiratory tract has ciliated cells that sweep mucus and trap particles up into the throat.
The stomach's acidic pH inhibits the growth of or kills many types of bacteria.
Normal bacteria in the large intestine and other areas prevent pathogens from taking up residence.
The Inflammatory Response
The inflammatory response is important in defending against pathogens.
Neutrophils and macrophages are used to surround and kill pathogens.
Protective proteins are also involved.
Four hallmark symptoms of inflammation are redness, heat, swelling, and pain.
Capillary changes in the damaged area cause the four signs of inflammation.
Chemical mediators, such as histamine, cause capillaries to dilate and become more permeable.
Increased blood flow brings white blood cells to the area.
Increased permeability of capillaries allows fluids and proteins to escape into tissues.
Clot formation in the injured area prevents blood loss.
Excess fluid in the area causes pain associated with swelling.
Neutrophils are the first to arrive and actively phagocytize debris, dead cells, and bacteria.
If neutrophils die off in great quantity, they become pus.
If neutrophils are overwhelmed, they call for reinforcements by secreting cytokines.
Cytokines attract more white blood cells to the area, including monocytes.
Monocytes become macrophages, even more, powerful phagocytes than neutrophils.
Inflammation is the body's natural response to irritation or injury.
Chronic inflammation can last for weeks, months, or even years.
Anti-inflammatory medications can minimize the effects of various chemical mediators.
The Complement System
The complement system is composed of blood plasma proteins designated by the letter C and a number.
Complement proteins complement certain immune responses, hence their name.
They amplify the inflammatory response by binding to mast cells and triggering histamine release.
They attract phagocytes to the site of infection.
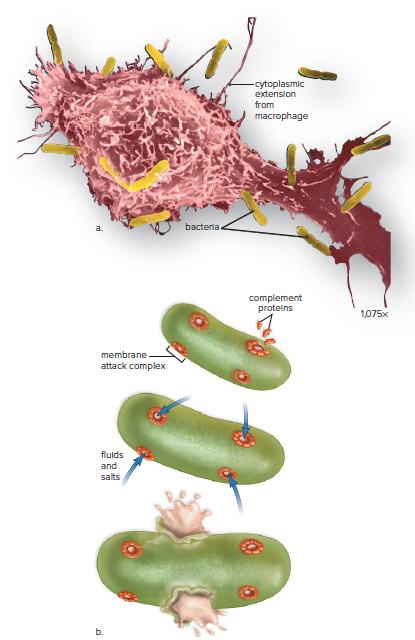
Some complement proteins bind to the surface of pathogens already coated with antibodies, ensuring their phagocytosis by neutrophils or macrophages.
Certain complement proteins join to form a membrane attack complex, which creates holes in the surfaces of microbes.
The membrane attack complex causes fluids and salts to enter the pathogen, leading to its bursting.
Natural Killer Cells
Natural killer (NK) cells are large, granular lymphocytes that kill virus-infected cells and tumor (cancer) cells by cell-to-cell contact.
NK cells attack and kill cells that have lost their ability to produce self-proteins.
Cells of the body have self-proteins on their surface that bind to receptors on NK cells.
When NK cells can't find self-proteins to bind to, they kill the cell using the same method as T lymphocytes.
NK cells are not specific, and their numbers do not increase when exposed to a particular antigen.
NK cells have no means of "remembering" an antigen from previous contact with it.
26.3 Specific Defenses and Adaptive Immunity
Nonspecific defenses are the first line of defense against infections.
If nonspecific defenses fail, specific defenses or adaptive immunity come into play.
Specific defenses respond to antigens, which may be components of a pathogen or cancer cell.
Antigens act as markers that a pathogen may be present in the body.
The immune system detects the marker and begins to actively look for cells that possess the antigen.
Lymphocytes are capable of recognizing antigens because their plasma membranes have receptor proteins.
B lymphocytes mature in the bone marrow and give rise to plasma cells, which produce antibodies.
T lymphocytes mature in the thymus and do not produce antibodies.
Some T lymphocytes regulate the immune response and other T lymphocytes directly attack cells that bear antigens.
Immunity usually lasts for some time and is primarily the result of the action of B and T lymphocytes.
The immune system is able to distinguish self from nonself to aid, rather than disrupt, homeostasis.

B Cells and the Antibody Response
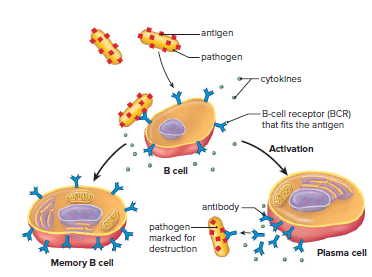
Each B cell can only bind to a specific antigen that fits the binding site of its receptor.
The receptor is called a B-cell receptor (BCR).
B cells are activated when an antigen binds to their BCR.
Activated B cells divide and produce many plasma cells and memory B cells.
This mechanism is called the clonal selection model.
B cells are stimulated by cytokines to divide and produce plasma cells.
Plasma cells have extensive rough endoplasmic reticulum for mass production and secretion of antibodies.
Antibodies produced by plasma cells are identical to the BCR of the activated B cell.
Memory B cells are responsible for long-term immunity.
Memory B cells quickly divide and give rise to more plasma cells capable of producing the correct antibodies if the same antigen enters the system again.
Once the threat of an infection has passed, the development of new plasma cells ceases, and those present undergo apoptosis.
The Function of Antibodies:
Antibodies are immunoglobulin proteins.
They can combine with a specific antigen.
The antigen-antibody reaction can produce antigen-antibody complexes.
These complexes mark the antigens for destruction.
The complexes can be engulfed by neutrophils or macrophages.
The complexes can activate the complement system.
The complement system makes the pathogens more susceptible to phagocytosis.
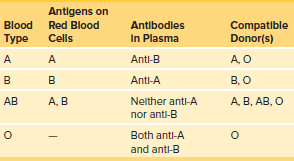
ABO Blood Type
Antibodies can be understood by examining human blood types.
Blood types are categorized as A, B, AB, or O based on antigens in red blood cells.
Type O blood has both anti-A and anti-B antibodies in the plasma.
Giving type A blood to a person with type O blood will cause agglutination.
Type O blood can be given to a person with any blood type.
Other red blood cell antigens are used in typing blood besides A and B.
The donor's blood should be put on a slide with the recipient's blood to determine compatibility.
T Cells and the Cellular Response
T cells have unique T-cell receptors (TCRs) when they leave the thymus, just like B cells.
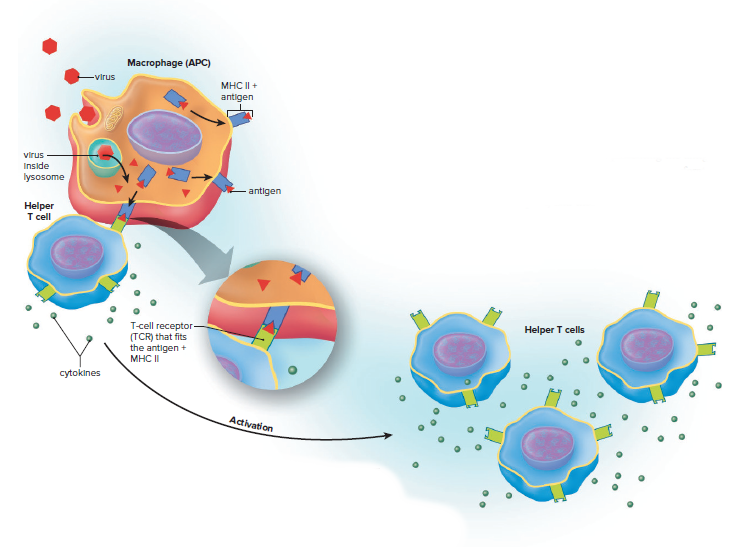
T cells require an antigen-presenting cell (APC) to recognize an antigen.
Macrophages become APCs by ingesting and destroying a pathogen.
The APC travels to a lymph node or spleen where T cells congregate.
An antigen from a virus is combined with a major histocompatibility complex (MHC) protein after being digested in a lysosome.
The MHC + antigen complex is presented to a T cell.
The two main types of T cells are helper T cells (TH cells) and cytotoxic T cells (TC cells).
TH cells recognize antigens presented by APCs with MHC class II molecules on their surface.
TC cells recognize antigens presented by APCs with MHC class I molecules on their surface.
Apoptosis contributes to homeostasis by regulating the number of cells present in the immune system.
T-cell cancers can result when apoptosis does not occur as it should.
T cells that have the potential to destroy the body's own cells undergo apoptosis in the thymus gland.

Functions of Cytotoxic T Cells and Helper T Cells
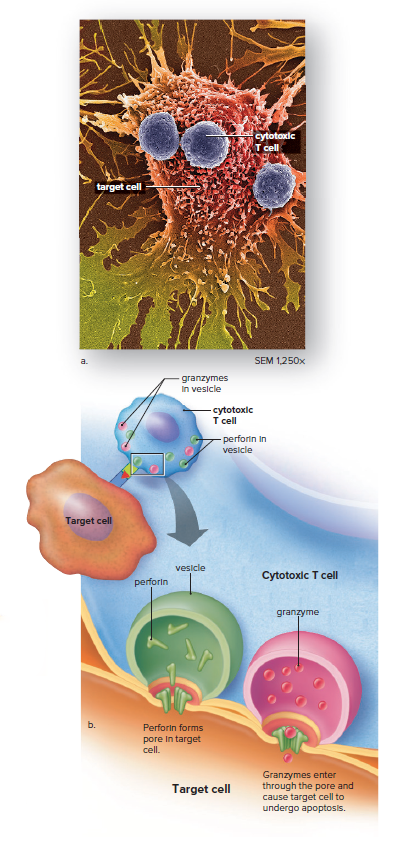
Cytotoxic T cells specialize in cell-to-cell combat.
They have storage vacuoles containing proteins called perforins or enzymes called granzymes.
When a cytotoxic T cell binds to a virus-infected or cancer cell presenting the antigen it has learned to recognize, it releases perforin molecules, which perforate the target cell’s plasma membrane, forming a pore.
The cytotoxic T cell then delivers a supply of granzymes into the pore, and these cause the cell to undergo apoptosis.
Once cytotoxic T cells have released their perforins and granzymes, they move on to the next target cell.
Cytotoxic T cells are responsible for a cellular response to virus-infected and cancer cells.
Helper T cells specialize in regulating immunity by secreting cytokines that stimulate B cells and cytotoxic T cells.
Cloned T cells include memory T cells that live for many years and can jumpstart an immune response to an antigen that was dealt with before.
HIV infects helper T cells and other cells of the immune system, inactivating the immune response and making HIV-infected individuals susceptible to opportunistic infections.
Infected macrophages serve as reservoirs for the HIV virus.
Tissue Rejection
Certain organs (skin, heart, kidneys) can be transplanted from one person to another if the body does not reject them.
Rejection occurs due to cytotoxic T cells and antibodies destroying foreign tissues in the body.
The immune system distinguishes between self and nonself when rejection occurs.
Organ rejection can be controlled by selecting the organ carefully and administering immunosuppressive drugs.
The transplanted organs should have the same type of MHC proteins as the recipient to avoid being antigenic to the recipient's T cells.
Immunosuppressive drugs inhibit T cell response to cytokines, weakening all types of immune responses.
26.4 Immunizations
After an infection, a person may become immune to it.
Childhood diseases like measles and mumps can provide lasting immunity.
Sexually transmitted diseases usually do not provide lasting immunity.
Vaccines are substances that stimulate the immune system without causing illness.
Vaccines can be made from pathogens or genetically engineered bacteria.
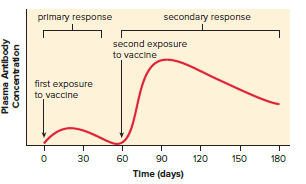
Immunization promotes active immunity, which is long-lasting.
Active immunity is dependent on memory B and T cells.
Passive immunity is temporary and can be obtained through prepared antibodies.
Newborns receive passive immunity from their mothers, but it soon disappears.
Gamma globulin injections can provide passive immunity but may cause serum sickness.
26.5 Disorders of the Immune System
The immune system protects us from disease by distinguishing self from nonself.
Sometimes, the immune system responds in a way that harms the body.
Allergies and autoimmune diseases are examples of harmful immune responses.
Allergies
Allergies are hypersensitivities to substances in the environment.
Allergens are substances that cause an immune reaction.
Immediate allergic responses are caused by receptors attached to the plasma membranes of mast cells in the tissues.
Mast cells release histamine and other substances that bring about the symptoms.
Anaphylactic shock is a severe reaction characterized by a sudden and life-threatening drop in blood pressure.
Allergy shots may prevent the onset of an allergic response.
Delayed allergic responses are probably initiated by memory T cells at the site of allergen contact in the body.
A classic example of a delayed allergic response is the skin test for tuberculosis (TB).
Contact dermatitis is also an example of a delayed allergic response.
Autoimmune Diseases
Autoimmune diseases occur when cytotoxic T cells or antibodies attack the body's own cells as if they were antigens.
The cause of autoimmune diseases is unknown, but they can sometimes occur after an individual has recovered from an infection.
Myasthenia gravis is an autoimmune disease that affects neuromuscular junctions, causing muscular weakness.
Multiple sclerosis (MS) is an autoimmune disease that causes the breakdown of the myelin sheath of nerve fibers, resulting in various neuromuscular disorders.
Systemic lupus erythematosus causes various symptoms prior to death due to kidney damage.
Rheumatoid arthritis affects the joints.
Rheumatic fever and type 1 diabetes are suggested to be autoimmune illnesses.
There are currently no cures for autoimmune diseases, but they can be controlled with drugs.
AIDS
AIDS is caused by HIV, which destroys helper T cells in the immune system.
Without helper T cells, the immune system can no longer fight off viruses, fungi, and bacteria.
Symptoms of AIDS include weight loss, chronic fever, cough, diarrhea, swollen glands, and shortness of breath.
HIV is transmitted through sexual contact, needle sharing, and from mother to child during birth or breastfeeding.
Advances in treatment have prolonged life, but new strains of the virus have emerged that are resistant to drugs.
AIDS vaccine trials are underway, but the process can take many years.
The human body's ability to suppress the infection keeps scientists hopeful that there is a way to help the body overcome HIV infection.
Suggestions for preventing HIV infection include abstaining from sexual intercourse, using a condom, and avoiding risky behavior such as intravenous drug use.
Chapter 26: Defenses Against Disease
26.1 Overview of the Immune System
The immune system fights infections and cancer to keep us healthy.
The immune system contains lymphatic organs such as the red bone marrow, thymus, lymph nodes, and spleen.
Lymphoid tissue can also be found in the tonsils and appendix.

Lymphatic Organs
Each of the lymphatic organs has a particular function in immunity, and each is rich in lymphocytes, one of the types of white blood cells.
Red Bone Marrow
Most bones in a child have red bone marrow
In an adult, red bone marrow is still present in certain bones:
Skull
Sternum (breastbone)
Ribs
Clavicle
Pelvic bones
Vertebral column
Ends of the humerus and femur nearest their attachment to the body
Red bone marrow produces all types of blood cells.
Lymphocytes differentiate into B lymphocytes (B cells) or T lymphocytes (T cells).
B lymphocytes are produced and mature in the bone marrow.
T lymphocytes mature in the thymus.
B lymphocytes produce antibodies.
T lymphocytes kill antigen-bearing cells outright.

Thymus
The thymus is soft and bilobed.
The size of the thymus varies and is larger in children.
The thymus shrinks as we get older.
The thymus plays a role in the maturing of T lymphocytes.
Immature T lymphocytes migrate from the bone marrow to the thymus.
T lymphocytes mature in the thymus.
Only 5% of T lymphocytes leave the thymus.
T lymphocytes that react with our own body die.
T lymphocytes that can attack foreign cells leave the thymus and enter lymphatic vessels and organs.
Lymph Nodes
Lymph nodes are small, ovoid structures along lymphatic vessels.
Lymph nodes filter lymph and keep it free of pathogens and antigens.
Lymph is filtered as it flows through a lymph node because the node’s many sinuses (open spaces) are lined by macrophages.
Macrophages are large, phagocytic cells that engulf and then devour as many as a hundred pathogens and still survive.
Lymph nodes contain many lymphocytes and are instrumental in fighting infections and cancer.
Some lymph nodes are located near the surface of the body and are named for their location.
For example, inguinal nodes are in the groin, and axillary nodes are in the armpits.
Physicians often feel for the presence of swollen, tender lymph nodes in the neck as evidence that the body is fighting an infection.
This method is a non-invasive, preliminary way to help them make a diagnosis.
Spleen
The spleen is located in the upper left abdominal cavity and is about the size of a fist.
The spleen filters the blood and contains red pulp and white pulp tissue.
The red pulp sinuses filter the blood of pathogens and debris, including worn-out red blood cells.
The white pulp contains lymphocytes that fight infections and cancer.
The spleen's outer capsule is thin and can burst due to infection or severe blow.
Other organs can fulfill the spleen's functions, but individuals without a spleen are more susceptible to infections.
People without a spleen may need to receive certain vaccinations and antibiotic therapy indefinitely.
Other Locations of Lymphoid Tissue
Tonsils and the appendix are lymphatic tissue structures.
Tonsils are located in the pharynx.
The appendix is attached to a portion of the large intestine.
Both tonsils and appendix belong to the immune system.
Cells of the Immune System
The immune system consists of lymphatic organs, lymphatic tissues, and various cells.
The cells in the immune system help distinguish between self and nonself cells.
Pathogens are identified by the presence of antigens, which are usually proteins or carbohydrates.
The immune system provides immunity by repelling foreign substances, pathogens, and cancer cells.
There are two levels of immunity: nonspecific immunity and specific (adaptive) immunity.
Nonspecific immunity repels pathogens indiscriminately, while specific immunity requires a certain antigen to be present.
26.2 Nonspecific Defenses and Innate Immunity
The body has innate immunity.
Innate immunity is composed of various types of nonspecific defenses.
Nonspecific defenses are the first line of defense against most types of infections.
Nonspecific defenses include:
Barriers to entry.
Inflammatory response.
Complement system.
Natural killer cells.
Barriers to Entry
Skin and mucous membranes in respiratory, digestive, reproductive, and urinary tracts act as mechanical barriers to pathogens.
Oil gland secretions contain chemicals that weaken or kill certain bacteria on the skin.
The upper respiratory tract has ciliated cells that sweep mucus and trap particles up into the throat.
The stomach's acidic pH inhibits the growth of or kills many types of bacteria.
Normal bacteria in the large intestine and other areas prevent pathogens from taking up residence.

The Inflammatory Response
The inflammatory response is important in defending against pathogens.
Neutrophils and macrophages are used to surround and kill pathogens.
Protective proteins are also involved.
Four hallmark symptoms of inflammation are redness, heat, swelling, and pain.
Capillary changes in the damaged area cause the four signs of inflammation.
Chemical mediators, such as histamine, cause capillaries to dilate and become more permeable.
Increased blood flow brings white blood cells to the area.
Increased permeability of capillaries allows fluids and proteins to escape into tissues.
Clot formation in the injured area prevents blood loss.
Excess fluid in the area causes pain associated with swelling.
Neutrophils are the first to arrive and actively phagocytize debris, dead cells, and bacteria.
If neutrophils die off in great quantity, they become pus.
If neutrophils are overwhelmed, they call for reinforcements by secreting cytokines.
Cytokines attract more white blood cells to the area, including monocytes.
Monocytes become macrophages, even more, powerful phagocytes than neutrophils.
Inflammation is the body's natural response to irritation or injury.
Chronic inflammation can last for weeks, months, or even years.
Anti-inflammatory medications can minimize the effects of various chemical mediators.

The Complement System
The complement system is composed of blood plasma proteins designated by the letter C and a number.
Complement proteins complement certain immune responses, hence their name.
They amplify the inflammatory response by binding to mast cells and triggering histamine release.
They attract phagocytes to the site of infection.
Some complement proteins bind to the surface of pathogens already coated with antibodies, ensuring their phagocytosis by neutrophils or macrophages.
Certain complement proteins join to form a membrane attack complex, which creates holes in the surfaces of microbes.
The membrane attack complex causes fluids and salts to enter the pathogen, leading to its bursting.

Natural Killer Cells
Natural killer (NK) cells are large, granular lymphocytes that kill virus-infected cells and tumor (cancer) cells by cell-to-cell contact.
NK cells attack and kill cells that have lost their ability to produce self-proteins.
Cells of the body have self-proteins on their surface that bind to receptors on NK cells.
When NK cells can't find self-proteins to bind to, they kill the cell using the same method as T lymphocytes.
NK cells are not specific, and their numbers do not increase when exposed to a particular antigen.
NK cells have no means of "remembering" an antigen from previous contact with it.
26.3 Specific Defenses and Adaptive Immunity
Nonspecific defenses are the first line of defense against infections.
If nonspecific defenses fail, specific defenses or adaptive immunity come into play.
Specific defenses respond to antigens, which may be components of a pathogen or cancer cell.
Antigens act as markers that a pathogen may be present in the body.
The immune system detects the marker and begins to actively look for cells that possess the antigen.
Lymphocytes are capable of recognizing antigens because their plasma membranes have receptor proteins.
B lymphocytes mature in the bone marrow and give rise to plasma cells, which produce antibodies.
T lymphocytes mature in the thymus and do not produce antibodies.
Some T lymphocytes regulate the immune response and other T lymphocytes directly attack cells that bear antigens.
Immunity usually lasts for some time and is primarily the result of the action of B and T lymphocytes.
The immune system is able to distinguish self from nonself to aid, rather than disrupt, homeostasis.

B Cells and the Antibody Response
Each B cell can only bind to a specific antigen that fits the binding site of its receptor.
The receptor is called a B-cell receptor (BCR).
B cells are activated when an antigen binds to their BCR.
Activated B cells divide and produce many plasma cells and memory B cells.
This mechanism is called the clonal selection model.
B cells are stimulated by cytokines to divide and produce plasma cells.
Plasma cells have extensive rough endoplasmic reticulum for mass production and secretion of antibodies.
Antibodies produced by plasma cells are identical to the BCR of the activated B cell.
Memory B cells are responsible for long-term immunity.
Memory B cells quickly divide and give rise to more plasma cells capable of producing the correct antibodies if the same antigen enters the system again.
Once the threat of an infection has passed, the development of new plasma cells ceases, and those present undergo apoptosis.

The Function of Antibodies:
Antibodies are immunoglobulin proteins.
They can combine with a specific antigen.
The antigen-antibody reaction can produce antigen-antibody complexes.
These complexes mark the antigens for destruction.
The complexes can be engulfed by neutrophils or macrophages.
The complexes can activate the complement system.
The complement system makes the pathogens more susceptible to phagocytosis.
ABO Blood Type
Antibodies can be understood by examining human blood types.
Blood types are categorized as A, B, AB, or O based on antigens in red blood cells.
Type O blood has both anti-A and anti-B antibodies in the plasma.
Giving type A blood to a person with type O blood will cause agglutination.
Type O blood can be given to a person with any blood type.
Other red blood cell antigens are used in typing blood besides A and B.
The donor's blood should be put on a slide with the recipient's blood to determine compatibility.

T Cells and the Cellular Response
T cells have unique T-cell receptors (TCRs) when they leave the thymus, just like B cells.
T cells require an antigen-presenting cell (APC) to recognize an antigen.
Macrophages become APCs by ingesting and destroying a pathogen.
The APC travels to a lymph node or spleen where T cells congregate.
An antigen from a virus is combined with a major histocompatibility complex (MHC) protein after being digested in a lysosome.
The MHC + antigen complex is presented to a T cell.
The two main types of T cells are helper T cells (TH cells) and cytotoxic T cells (TC cells).
TH cells recognize antigens presented by APCs with MHC class II molecules on their surface.
TC cells recognize antigens presented by APCs with MHC class I molecules on their surface.
Apoptosis contributes to homeostasis by regulating the number of cells present in the immune system.
T-cell cancers can result when apoptosis does not occur as it should.
T cells that have the potential to destroy the body's own cells undergo apoptosis in the thymus gland.


Functions of Cytotoxic T Cells and Helper T Cells
Cytotoxic T cells specialize in cell-to-cell combat.
They have storage vacuoles containing proteins called perforins or enzymes called granzymes.
When a cytotoxic T cell binds to a virus-infected or cancer cell presenting the antigen it has learned to recognize, it releases perforin molecules, which perforate the target cell’s plasma membrane, forming a pore.
The cytotoxic T cell then delivers a supply of granzymes into the pore, and these cause the cell to undergo apoptosis.
Once cytotoxic T cells have released their perforins and granzymes, they move on to the next target cell.
Cytotoxic T cells are responsible for a cellular response to virus-infected and cancer cells.
Helper T cells specialize in regulating immunity by secreting cytokines that stimulate B cells and cytotoxic T cells.
Cloned T cells include memory T cells that live for many years and can jumpstart an immune response to an antigen that was dealt with before.
HIV infects helper T cells and other cells of the immune system, inactivating the immune response and making HIV-infected individuals susceptible to opportunistic infections.
Infected macrophages serve as reservoirs for the HIV virus.

Tissue Rejection
Certain organs (skin, heart, kidneys) can be transplanted from one person to another if the body does not reject them.
Rejection occurs due to cytotoxic T cells and antibodies destroying foreign tissues in the body.
The immune system distinguishes between self and nonself when rejection occurs.
Organ rejection can be controlled by selecting the organ carefully and administering immunosuppressive drugs.
The transplanted organs should have the same type of MHC proteins as the recipient to avoid being antigenic to the recipient's T cells.
Immunosuppressive drugs inhibit T cell response to cytokines, weakening all types of immune responses.
26.4 Immunizations
After an infection, a person may become immune to it.
Childhood diseases like measles and mumps can provide lasting immunity.
Sexually transmitted diseases usually do not provide lasting immunity.
Vaccines are substances that stimulate the immune system without causing illness.
Vaccines can be made from pathogens or genetically engineered bacteria.
Immunization promotes active immunity, which is long-lasting.
Active immunity is dependent on memory B and T cells.
Passive immunity is temporary and can be obtained through prepared antibodies.
Newborns receive passive immunity from their mothers, but it soon disappears.
Gamma globulin injections can provide passive immunity but may cause serum sickness.

26.5 Disorders of the Immune System
The immune system protects us from disease by distinguishing self from nonself.
Sometimes, the immune system responds in a way that harms the body.
Allergies and autoimmune diseases are examples of harmful immune responses.
Allergies
Allergies are hypersensitivities to substances in the environment.
Allergens are substances that cause an immune reaction.
Immediate allergic responses are caused by receptors attached to the plasma membranes of mast cells in the tissues.
Mast cells release histamine and other substances that bring about the symptoms.
Anaphylactic shock is a severe reaction characterized by a sudden and life-threatening drop in blood pressure.
Allergy shots may prevent the onset of an allergic response.
Delayed allergic responses are probably initiated by memory T cells at the site of allergen contact in the body.
A classic example of a delayed allergic response is the skin test for tuberculosis (TB).
Contact dermatitis is also an example of a delayed allergic response.
Autoimmune Diseases
Autoimmune diseases occur when cytotoxic T cells or antibodies attack the body's own cells as if they were antigens.
The cause of autoimmune diseases is unknown, but they can sometimes occur after an individual has recovered from an infection.
Myasthenia gravis is an autoimmune disease that affects neuromuscular junctions, causing muscular weakness.
Multiple sclerosis (MS) is an autoimmune disease that causes the breakdown of the myelin sheath of nerve fibers, resulting in various neuromuscular disorders.
Systemic lupus erythematosus causes various symptoms prior to death due to kidney damage.
Rheumatoid arthritis affects the joints.
Rheumatic fever and type 1 diabetes are suggested to be autoimmune illnesses.
There are currently no cures for autoimmune diseases, but they can be controlled with drugs.
AIDS
AIDS is caused by HIV, which destroys helper T cells in the immune system.
Without helper T cells, the immune system can no longer fight off viruses, fungi, and bacteria.
Symptoms of AIDS include weight loss, chronic fever, cough, diarrhea, swollen glands, and shortness of breath.
HIV is transmitted through sexual contact, needle sharing, and from mother to child during birth or breastfeeding.
Advances in treatment have prolonged life, but new strains of the virus have emerged that are resistant to drugs.
AIDS vaccine trials are underway, but the process can take many years.
The human body's ability to suppress the infection keeps scientists hopeful that there is a way to help the body overcome HIV infection.
Suggestions for preventing HIV infection include abstaining from sexual intercourse, using a condom, and avoiding risky behavior such as intravenous drug use.
 Knowt
Knowt